|
|
Head: Prof. Vladimír Holáň, PhD, DScE-mail: holan@biomed.cas.cz |
The department is primarily focused on the study of cellular and molecular mechanisms specific to transplantation immunity and to use this knowledge in the regulation of immune responses. The aim is to improve the survival of genetically diverse cells and tissue transplants.
The basic model proposed involves the use of cultured and specifically differentiated stem cells (mesenchymal, limbic), which are transplanted with different kinds of nanofiber media for the purpose of repairing severe damage to the skin and ocular surface as well as replenishing limbal stem cell deficiencies. It uses a wide range of methods of cell and molecular biology, such as cell cultures, differentiation of stem cells, the study of gene regulation (PCR, real time PCR), the production and detection of cytokines using assays(ELISA, ELISPOT), flow cytometry, MACS, Western blotting, experimental models of transplantation of skin, cornea, limbus, and stem cell transfers.Themain objective is to test the knowledge gained in preclinical models and their potential use in clinical practice (particularly in patients with severe ocular surface wounds).
|
Research Scientist: Prof. Vladimír Holáň, PhD, DSc
PhD Students:
Undergraduate Students: Pavla Boháčová Jan Kössl
Technicans: |
Research topics
The transplantation of an organ or the transfer of stem cells often represents the only way to improve or even to rescue the life of a patient. However, immunological rejection represents a major obstacle to the further development of therapeutic transplantation. Therefore, deep knowledge of the molecular and cellular mechanisms of the transplantation reaction is required. Using a model of immunological reaction to histocompatibility antigens, we have focused our research on studying the activation and function of regulatory T cells in transplantation immunity and tolerance. Using a model of orthotopic corneal and limbal transplantation, we have analyzed the details of ocular immunity. Since successful treatment of the severely damaged ocular surface requires the transfer of limbal stem cells, we recently started to isolate, grow and characterize stem cells. We succeeded in isolating limbal and mesenchymal stem cells in the mouse and using them for the repair of the damaged corneal epithelium. For the transfer of stem cells, we use various types of nanofibre scaffolds, which represent optimal 3D matrices for stem cell growth. Well-established methods for monitoring the immune response enabled us, in co-operation with other laboratories, to study the cytokine response in various experimental models of immunoregulation. The ultimate goal of our research is to acquire insights into the mechanisms of the specific immune response, to isolate and transplant stem cells and to propose novel strategies for targeted immunoregulation.
Recent experiments have also been focused on the targeted differentiation of mesenchymal stem cells in vitro and their use for ocular surface reconstruction. This is one of our models for testing the possibilities of using stem cell transplantation in regenerative and reparative medicine.
|
Fig. 1: Experimental model of skin grafting in inbred strains of mice. Skin allografts in mice are protected by bandages for 10 days, then the survival of the grafts in immunomodulated recipients is monitored and evaluated.
|
|
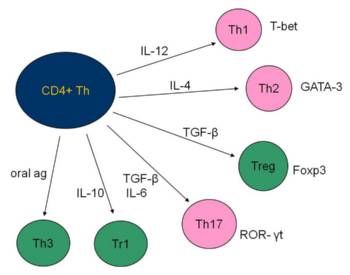
Fig. 2: The scheme of the regulatory role of cytokines in the development of individual phenotypically and functionally distinct subpopulations of T lymphocytes.
|
|
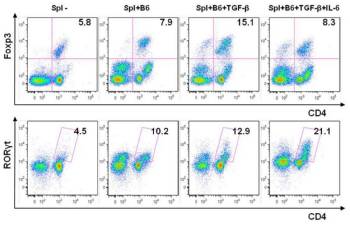
Fig. 3: Flow cytometry analysis of the in vitro induction and development of regulatory T lymphocytes and proinflammatory Th17 cells. Spleen cells from BALB/c mice were cultured with irradiated cells from B6 mice in the absence or presence of the determining cytokines TGF-ß and IL-6, and the percentage of regulatory T cells (Foxp3+ cells) or Th17 cells (RORγt+ cells) was determined by FACS analysis.
|
|
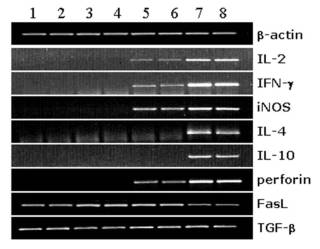
Fig. 4: Expression of genes for immunologically relevant molecules in rejected corneal allografts and xenografts in an experimental mouse model. Corneal grafts were transplanted orthotopically, and the expression of genes for the tested molecules was detected in individual corneas by PCR. Lanes 1,2 – healthy cornea, 3,4 – corneal autografts, 5.6 – corneal allografts, 7,8 – corneal xenografts.
|
Významné výsledky oddělení v roce 2013
1. Regeneration of severely damaged ocular surface by stem cells
Limbal and mesenchymal stem cells were cultured in vitro on nanofiber scaffolds and transferred on the damaged ocular surface in experimental animal models. The therapeutic effects of stem cells were evaluated by histology and according to the ability to inhibit expresssion of genes for proinflammatory molecules IL-2, IFN-gama, IL-17 and iNOS. The results thus demonstrate the ability of stem cells and nanofiber scaffolds to regenerate ocular surface after the injury.
Collaboration: Evropská oční klinika Lexum, Praha.
|
|
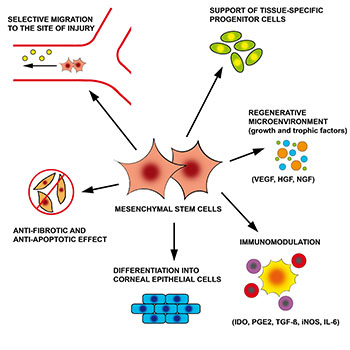
A scheme of immunoregulatory and therapeutic effects of mesenchymal stem cells. There are number of diferent mechanisms by which MSC contribute to the healing process. Differentiation into epithelial-like cells, immunomodulation and the production of growth and trophic factors are the most important mechanisms. |
|
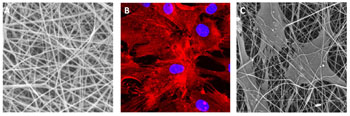
A structure of nanofiber scaffold (A) and the growth of mesenchymal stem cells on nanofiber scaffold (B, C). (A) Scanning electron microscopy image of nanofibers from copolymer polyamid 6/12, the avarage nanofiber diameter is 380 nm, (B) Mouse MSC growing on nanofibers (red filaments – F-actin stained with phalloidin, blue – DAPI staining of the nuclei), (C) Scanning electron microscopy of mouse MSC growing on nanofibers.
|
|
|
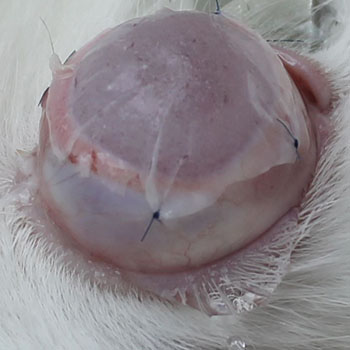
Chemically damaged eye of the rabbit covered by a nanofiber scaffold with stem cells. The application of a nanofiber scaffold seeded with MSC onto the damaged ocular surface of a rabbit.
|
Publications:
- Holáň, V., Javorková, E.: (2013) Mesenchymal stem cells, nanofiber scaffolds and ocular surface reconstruction. Stem Cells Rev. Rep. 9(5), 609-619. IF 4.523
- Čejková J., Tošan P., Čejka Č., Lenčová A., Zajícová A., Javorková E., Kubinová Š., Syková E., Holáň V.: (2013) Suppression of alkali-induced oxidative injury to the cornea by mesenchymal stem cells growing on nanofiber scaffolds and transferred onto the damaged corneal surface. Exp. Eye Res. 116, 312-323. IF 3.026
- Holáň, V., Javorková, E., Trošan, P.: The growth and delivery of mesenchymal and limbal stem cells using copolymer polyamide 6/12 nanofiber scaffolds. In: Wright, B. and Connon, C. J. (eds), Corneal Regenerative Medicine, Methods Mol. Biol., Humana Press – Springer, New York, London 2013, S. 187-199. ISBN 978-1-62703-431-9.
2. Distinct roles of cytokines in the development of regulatory T cells and regulatory B cells
The role of cytokines in development of regulatory T (Treg) and B (Breg) cells was described. TGF-beta was shown as the main cytokine determining the development of Tregs, but this cytokine inhbited activation of IL-10-producing Breg. On the contrary, another two cytokines, IL-12 and IFN-gama, enhanced the development of Breg. These results show distinct roles of cytokines in development of Treg and Breg, and suggest new approaches for targeted regulation of the immune system.
Collaboration: Přírodovědecká fakulta UK, Praha
|
|
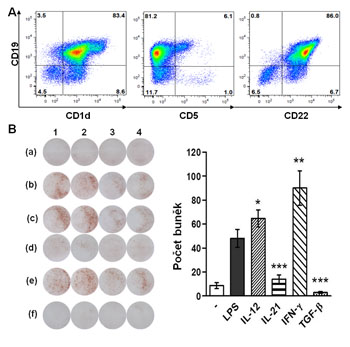
(A) Characterization of B cell populations by flow cytometry. (B) Detection of cells producing IL-10 using technology ELISPOT.
|
Publications:
- Holáň, V., Zajícová, A., Javorková, E., Trošan, P., Chudičková, M., Pavlíková, M., Krulová, M.: (2013) Distinct cytokines balance the development of regulatory T cells and IL-10-producing regulatory B cells. Immunology. In press. IF 3.705
- Kubera M., Curzytek K., Duda W., Leskiewicz M., Basta-Kaim A., Budziszewska B., Roman A., Zajícová A., Holáň V., Szczesny E., Lason W., Maes M.:. (2013) A new animal model of (chronic) depression induced by repeated and intermittent lipopolysaccharide administration for 4 months. Brain Behav. Immun. 31, 96-104. IF 5.612
- Holáň, V., Krulová, M.: (2013) Common and small molecules as the ultimate regulatory and effector mediators of antigen-specific transplantation reactions. World J. Transplant. 3(4), 54-61. (nový časopis, zatím bez IF)